CASE REPORT | https://doi.org/10.5005/jp-journals-10082-02237 |
Systemic Lupus Erythematosus in a Man with Unusual Combination of Multiple Antibodies: A Rare Presentation
1Titoria’s Clinics, Noida, Uttar Pradesh, India
2Department of Dermatology, Venereology and Leprosy, Believers Church Medical College, Thiruvalla, Kerala, India
Corresponding Author: Roshni Kakitha, Titoria’s Clinics, Noida, Uttar Pradesh, India, Phone: +91 7708541823, e-mail: k.roshni55@gmail.com
How to cite this article Kakitha R, Ambujam S. Systemic Lupus Erythematosus in a Man with Unusual Combination of Multiple Antibodies: A Rare Presentation. J Basic Clin Appl Health Sci 2020;3(3):131–132.
Source of support: Nil
Conflict of interest: None
ABSTRACT
Systemic lupus erythematosus (SLE) is a connective tissue disorder involving multiple systems of the body, skin being one of the earliest systems to get involved. We report the case of a 29-year-old male patient, with acute vesicular malar rash and a host of positive antibodies, viz., ANA, anti-ds DNA, anti-Smith, APAbs, anti-U1RNP, and anti-histone. He also had low complement levels. Occurrence of SLE is rare in men. Presence of a variety of antibodies without the correlating systemic involvement is rarer still, making this a case worth reporting.
Keywords: Antibodies, Complement, Men, Systemic lupus erythematosus.
INTRODUCTION
Systemic lupus erythematosus (SLE) is an autoimmune inflammatory condition involving multiple organs including the skin. The clinical presentation is variable and greatly depends on the specific organs involved and severity of the disease.1 It is associated with multiple immunological abnormalities.1
The American College of Rheumatology (ACR) criteria, or the more recent Systemic Lupus International Collaborating Clinics (SLICC) criteria, are used to diagnose it.1
CASE DESCRIPTION
We report a 29-year-old man who presented with pain of finger joints of both hands and knee joints and intermittent fever for the last 6 months, as well as vesicles over sun-exposed areas of face and forearms of 2 months’ duration. He also gave a history of painless oral ulcers primarily of the palate. He had no history suggestive of vasculitic skin lesions or any peripheral vascular disease. He was breathless even on doing accustomed work. There was no history of intake of any lupus-inducing drugs like hydralazine, procainamide, quinidine, and isoniazid prior to the onset of skin lesions.
The examination revealed vesicles on erythemato-pigmented plaques of the sun-exposed areas of the skin of the face (Fig. 1), v area of the neck, front of chest (Fig. 2), extensor forearms (Fig. 3), and back (Fig. 4). He also had swollen finger joints (Fig. 5) and diffuse alopecia of the scalp. The oral mucosa had palatal erosions. A provisional diagnosis of SLE was made. Immunological tests were positive for a variety of antibodies (listed below). Renal biopsy showed diffuse segmental proliferative glomerulonephritis with the focal cellular crescents pattern [score/grade-ISN/RPS class IV S (A)]. Cardiovascular and central nervous system involvement was ruled out. Thus, a final diagnosis of SLE was made applying the relevant diagnostic criteria of both ACR and SLICC.

Fig. 1: Vesicles and erythemato-pigmented plaques on the face
Results of investigations done:
| Total count | 3600 cell/mm3 |
| ESR | 90 mm |
| 24-hour urine protein | 9.68 g |
| ANA | Positive |
| dsDNA | Positive |
| Sm antibody | Positive 166.95 RU/mL positive (≥20+) |
| U1-SnRNP | Positive 44 U/mL (>10+) |
| Histone antibody | Positive 96.96 U/mL positive (≥20+) |
| APLA | Positive |
| C3 | Reduced 44 mg/dL (90–180) |
| C4 | Reduced <6.65 mg/dL (10–40) |
| Serology for HIV/HBsAg | Negative |
| ECG/EEG/CXR | Normal |
| DC/LFT/RFT/electrolytes | Within normal limits |
| CRP/RF | Negative |

Fig. 2: Vesicles and erosions on the front of chest

Fig. 3: Vesicles on the sun-exposed areas on the forearm

Fig. 4: Vesicles and crusted erosions on the back
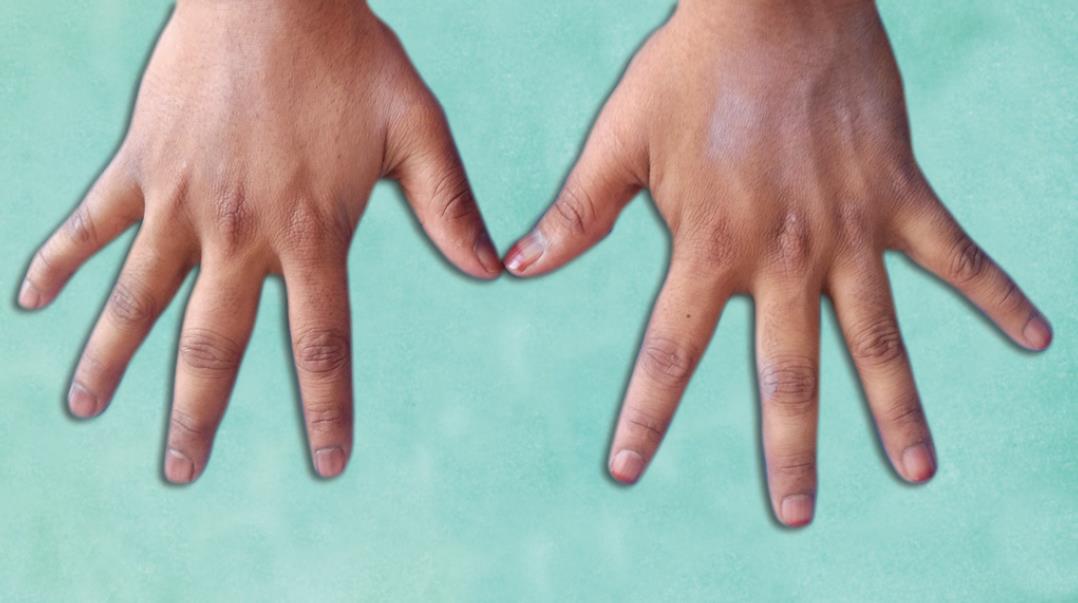
Fig. 5: Swelling of the joints of the fingers
The direct immunofluorescence study of the skin was not done since the other tests were conclusive for the diagnosis of SLE.1
Renal biopsy showed diffuse segmental proliferative glomerulonephritis with the focal cellular crescent pattern confirming lupus nephritis.
The patient responded to immunosuppressive treatments that included tapering doses of tablet methyl prednisolone, tablet hydroxychloroquine 200 mg BD, monthly cyclophosphamide pulse therapy, and topical sunscreens. The patient comes for regular follow-up to the nephrology and dermatology OPDs and has been in remission since then.
DISCUSSION
Systemic lupus erythematosus is not so common a disease where females outnumber males (approximately 7–15:1).1
Men with lupus tend to have higher frequencies of renal disease, skin manifestations, cytopenias, serositis, neurological involvement, thrombosis, and vasculitis.1
Our patient was diagnosed to have SLE based on both ACR and SLICC criteria, with histopathological confirmation of lupus nephritis [diffuse segmental proliferative glomerulonephritis with focal cellular crescents pattern, Score/grade-ISN/RPS class IV S (A)]. He was positive for anti-histone antibodies, though there was no history of intake of SLE-inducing drugs. In the absence of clinical mixed connective tissue disease, U1 SnRNP too was positive. He had low C3 levels, which is considered an independent predictor of severe lupus flare.1
Thus, our patient had an unusual combination of multiple specific and nonspecific antibodies without the clinical manifestations of some of them.
The following are the approximate frequencies of positivity in SLE:
| ANA | 98%1 (using Hep 2 cells) |
| dsDNA | 60–70%1 (Farr technique) |
| Sm antibody | 30%1 |
| U1-SnRNP | 23–40%1 |
| Histone antibody | 50% (including drug induced)2 |
| APLA | 15–34%1 |
| Hypocomplementemia | 62%3,4 |
The patient was positive for all the above antibodies.
This case is hence being reported as it is SLE in a male and also because of the combination of uncommon positive immunological tests.
Does this indicate a future turn of the disease for the worse, its evolution into an overlap, or yet another connective tissue disease? These are the questions that came to our mind.
REFERENCES
1. Rook’s Textbook of Dermatology, In: Griffiths C, Barker J, Bleiker T, Chalmers R, Creamer DChichester, West Sussex, Hoboken, NJ: John Wiley and Sons Inc; 2016.
2. Satoh M, Fritzler MJ, Chan EKL. Chapter 28—Antihistone and antispliceosome antibodies. In: ed. GC. Tsokos Systemic Lupus Erythematosus. Academic Press; 2021. pp. 237–247.
3. Abu-Shakra M, Gladman DD, Urowitz MB, Farewell V. Anticardiolipin antibodies in systemic lupus erythematosus: clinical and laboratory correlations. Am J Med 1995;99(6):624–628. DOI: 10.1016/S0002-9343(99)80249-6.
4. Ramos-Casals M, Campoamor MT, Chamorro A, Salvador G, Segura S, Botero JC, et al. Hypocomplementemia in systemic lupus erythematosus and primary antiphospholipid syndrome: prevalence and clinical significance in 667 patients. Lupus 2004;13(10):777–783. DOI: 10.1191/0961203304lu1080oa.
________________________
© The Author(s). 2020 Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by-nc/4.0/), which permits unrestricted use, distribution, and non-commercial reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.