|
CASE REPORT |
https://doi.org/10.5005/jp-journals-10082-03144
|
Complete Temporomandibular Joint Ankylosis with Nil Mouth Opening: An Anesthetic Challenge
1,2Department of Anaesthesia, Shri Sathya Sai Medical College and Research Institute, Chennai, Tamil Nadu, India
Corresponding Author: P Akshara, Department of Anaesthesia, Shri Sathya Sai Medical College and Research Institute, Chennai, Tamil Nadu, India, Phone: +91 8248392808, e-mail: drp.akshara@gmail.com
How to cite this article: Akshara P, Govindan DK. Complete Temporomandibular Joint Ankylosis with Nil Mouth Opening: An Anesthetic Challenge. J Basic Clin Appl Health Sci 2022;5(2):49–51.
Source of support: Nil
Conflict of interest: None
ABSTRACT
Securing an airway in pediatric patients with TMJ ankylosis with nil mouth opening is an anesthetic challenge. Among the methods available including submandibular intubation, retrograde intubation and tracheostomy, fiberoptic nasotracheal intubation technique remains gold standard. Self-awareness and calmness are important attributes of an anaesthetist during such cases. Prior planning of the anesthetic technique and good rapport with surgeon are of key importance for successful outcomes of such difficult airway cases. We present a case of Right Temporomandibular Joint Ankylosis for surgery in a pediatric age-group with nil mouth opening managed successfully with fiberoptic bronchoscope.
Keywords: Airway in TMJ ankylosis, Nil mouth opening, Pediatric difficult airway.
INTRODUCTION
The anesthetic management of paediatric airway with restricted or nil mouth opening due to temporomandibular joint ankylosis is a backbreaking task for anesthesiologist. Technically it encompasses both: management of paediatric patients, and difficult airway scenario.1 We present a case of right Right Temporomandibular Joint Ankylosis for surgery in a pediatric age-group with nil mouth opening managed successfully with fiberoptic bronchoscope.2
CASE DESCRIPTION
We present a case of a 6-year-old girl who weighed 18 kg and presented with chief complaints of inability to open mouth for the past 3 years. She had undergone surgery for right inflammatory myofibroblastic tumour 5 years before (scar of the surgery shown in Fig. 1), after which her mouth opening started decreasing progressively, resulting in nil mouth opening at the time of presentation as shown in Figure 2. The child was alert, conscious, oriented to time, place and person. Due to poor oral intake, her weight percentile was on a lower level when compared to children of her age. Vitals were appropriate for age, RS and CVS examination were normal. All biochemical investigations were within normal limits.
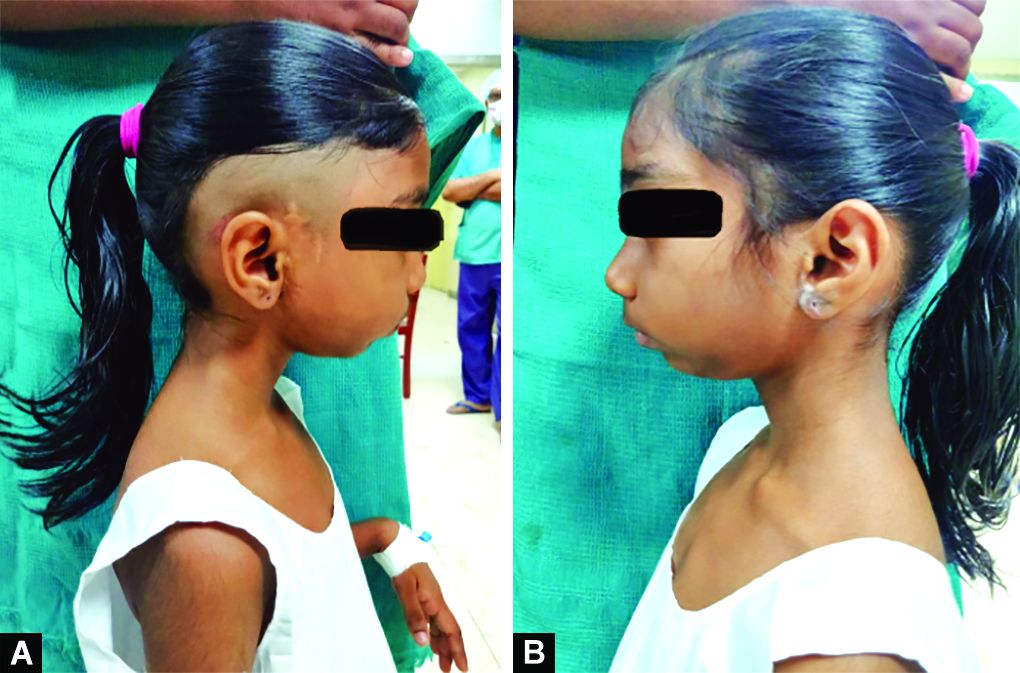
Figs 1A and B: Shows the difference between right ankylosed side (surgical scar present) and left normal side

Fig. 2: NIL mouth opening with absent upper incisors
AIRWAY ASSESSMENT
Mandibular subluxation test: Right condylar movement not palpable, left condylar movement midly palpable. Mouth opening was severily restricted. Upper central incisors were missing. Facial deformity with retrognathia and facial flattening present on the right side. Normal range of neck movements present. Computed tomography (CT) skull shows fusion of right mandibular condyl with glenoid fossa on whereas such fusion is absent on left side as seen in Figure 3.

Fig. 3: Scan showing fusion mandibular condyl with glenoid fossa on right side whereas such fusion is absent on left side
DISCUSSION
After shifting the patient inside OT, standard ASA monitors connected, adequate premedication with IV glycopyrrolate 0.04 mg/kg, IV hydrocortisone 2 mg/kg and IV dexamethasone 0.1 mg/kg IV and IV fentanyl 0.5 µg/kg were given.3,4 We used sevoflurane, nitrous oxide and oxygen along with topical anesthesia—lignocaine 2% nebulization. B/L nostril was prepped with 0.5% xylometazoline drops. Plan of anaesthesia was fiberoptic nasotracheal intubation which was done by rail loading the appropriately sized endotracheal tube over fiberoptic scope as one assembly. During this process anaesthesia was maintained by inserting (cut) 4 mm sized ETT into the other nostril as seen in Figures 4 and 5.5 Bolus dose of Propofol 20 mg given at the time of ETT tube insertion after visualization of vocal cords. Confirmation of endotracheal intubation was done by auscultation and visualization of end-tidal CO2 trace on capnograph. Anaesthesia was maintained with O2, N2O, sevoflurane, and IV atracurium with controlled ventilation. The surgeon confirmed mouth opening of two fingers at the end of surgery. The child was reversed after she regained spontaneous breathing and extubated when fully awake with intact airway reflexes. Extubation and postoperative period was uneventful. Postoperative pain was managed by intravenous paracetomol 15 mg/kg given every 8th hour.6,7

Fig. 4: Maintaining oxygenation in spontaneously breathing child by passing smaller size ETT tube as an alternate to nasopharyngeal airway in left nostril as a conduit

Fig. 5: Insertion of railroaded fibreoptic bronchoscope (FOB)
CONCLUSION
Pediatric difficult airway can be managed with ease if there is good planning and readiness to tackle any complications that arises. We conclude that a well lubricated smaller size ETT inserted after induction not only helps to maintain anaesthesia for fiberoptic bronchoscopy by giving enough time for its use but also helps to achieve adequate oxygenation and depth of anaesthesia.
ORCID
P Akshara http://orcid.org/0000-0002-5924-550X
Dilip K Govindan https://orcid.org/0000-0003-2597-1922
REFERENCES
1. Goswami D, Singh S, Bhutia O, Baidya D, Sawhney C. Management of young patients with temporomandibular joint ankylosis—a surgical and anesthetic challenge. Indian J Surg 2016;78(6):482–489. DOI: 10.1007/s12262-016-1551-5.
2. Sharma A, Dwivedi D, Sharma RM. Temporomandibular joint ankylosis: “A pediatric difficult airway management”. Anesth Essays Res 2018;12(1):282. DOI: 10.4103/aer.AER_122_17.
3. The Merck manual-home edition, Sec 8, Ch 96. Disorders of the Temporomandibular Joint.html.
4. Manganello-Souza LC, Mariani PB. Temporomandibular joint ankylosis: report of 14 cases. Int J Oral Maxillofac Surg 2003;32(1):24–29. DOI: 10.1054/ijom.2002.0308.
5. Garcia-Aparicio L, Parri FJ, Sancho MA, Sarget R, Morales L. Temporomandibular joint ankylosis (TMA) in children. Cir Pediatr 2000;13(2):62–63. PMID: 12602004.
6. Kobayashi R, Utsunomiya T, Yamamoto H, Nagura H. Ankylosis of the temporomandibular joint caused by rheumatoid arthritis: a pathological study and review. J Oral Sci 2001;43(2):97–101. DOI: 10.2334/josnusd.43.97.
7. Baykul T, Aydin MA, Nasir S. Avascular necrosis of the mandibular condyle causing fibrous ankylosis of the temporomandibular joint in sickle cell anemia. J Craniofac Surg 2004;15(6):1052–1056. DOI: 10.1097/00001665-200411000-00035.
________________________
© The Author(s). 2022 Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by-nc/4.0/), which permits unrestricted use, distribution, and non-commercial reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.